This page is intended to help Medical Elective students understand the risks and mitigation associated with being exposed to various diseases while working with patients. We do everything in our power to protect the health and welfare of our students.
HIV/AIDS
AIDS and HIV infection does occur worldwide. HIV is sometimes seen as being disease of the poor. In Africa there is some correlation between extreme poverty and high HIV prevalence, although HIV is prevalent across all sectors of society.
The Risks
Both men and women can become infected and can give the virus to someone else. HIV is passed from one person to another through blood-to-blood and sexual contact with someone who is infected with HIV. Also, an HIV-infected woman can pass the virus to her baby during pregnancy or during birth as well as through breastfeeding.
Rape plays a significant role in the high prevalence of HIV among women. Although HIV prevention campaigns encourage people to use condoms and have fewer sexual partners, women and girls in Africa are often unable to negotiate safer sex.
Factors to consider in assessing risk include the extent of direct contact with blood or other potentially infectious secretions and the extent of sexual contact with potentially infected persons or with persons whose HIV infection status is unknown.
Many persons may be infected and be unaware of their status. Therefore, if you engage in sexual contact, you may be unknowingly at risk from an infected sex partner.
Assess and take ownership of your personal behaviours; do not choose high-risk behaviours.
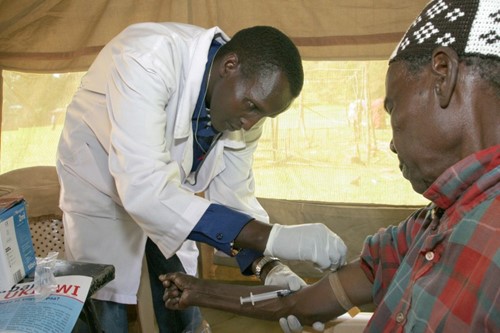
We always practise safe health measures when working with patients.
HIV can NOT be spread in the following ways:
× Shaking hands, hugging, or casual kissing
× Coughs or sneezes, sweat or tears
× Mosquitoes, toilet seats, door knob, drinking fountain
× Eating food prepared or handled by an infected person
× Everyday contact with HIV-infected persons at school, work, home or anywhere else.
Precautions
- Students should avoid use of unscreened blood-clotting factor concentrates or concentrates of uncertain purity. If transfusion is necessary, the blood should be tested, if possible, for HIV antibody by appropriately trained laboratory technicians using a reliable test.
- Students with insulin-dependent diabetes, haemophilia, or other conditions that necessitate routine or frequent injections are advised to carry a supply of syringes, needles, and disinfectant swabs (e.g., alcohol wipes) sufficient to last their entire stay abroad. Before travelling, students must request documentation of the medical necessity for travelling with these items (e.g., a doctor’s letter) in case official inspection personnel at ports of departure/entry question their need.
- Exercise caution at all times to avoid serious accidents or injuries that could require a blood transfusion.
- Abstinence is the only certain choice for preventing infection with HIV
- Exercise appropriate precautions if engaging in activities that expose you to risk of infection.
- All medical students working in high risk areas should wear appropriate equipment at all times, gloves, aprons and take the appropriate universal precautions at all times.
- Should an incident occur in which you suspect you were exposed to HIV, you should immediately seek immediate medical assistance, do not delay as the first 72 hours are critical.
- Consider taking a PEP treatment with you on your visit which can be available through your university.
PARASITIC INFECTION
The Risks
All freshwater in southern and sub-Saharan Africa–including the great lakes and rivers as well as smaller bodies of water–is considered to be at risk for schistosomiasis (a disease caused by parasitic worms’ transmission).
Infection occurs when skin comes in contact with contaminated freshwater in which certain types of snails that carry schistosomes are living.
Schistosoma parasites can penetrate the skin of persons who are wading, swimming, bathing, or washing in contaminated water. Within several weeks, worms grow inside the blood vessels of the body and produce eggs. Some of these eggs travel to the bladder or intestines and are passed into the urine or stool.
Occasionally, eggs may be deposited in the brain or spinal cord, leading to seizures or paralysis. More than 200 million people are infected worldwide.
If skin comes in contact with freshwater from canals, rivers, streams, or lakes, there is a risk of getting schistosomiasis.
No vaccine is available.
No drugs for preventing infection are available.
Untreated piped water coming directly from freshwater sources may contain cercariae larvae.
Precautions
- Do not wade or swim in freshwater in Southern African countries.
- Drink safe water. Because there is no way to make sure that water coming directly from canals, lakes, rivers, streams or springs is safe, you should either boil water for 1 minute or
- filter water before drinking it. Boiling water for at least 1 minute will kill any harmful parasites, bacteria, or viruses present.
- Brush your teeth with clean water.
- If you wear gas-permeable contacts use only clean water to rinse them.
- If you accidentally come into contact with fresh water, vigorous towel drying after a very brief water exposure may help to prevent the Schistosoma parasite from penetrating the skin.
The scope of the guidance below
This information below contains guidance on measures to protect clinical healthcare workers (HCWs) against occupational infection with blood-borne viruses (BBVs). It is based on the recommendations of the Expert Advisory Group on AIDS and the Advisory Group on Hepatitis.
This document covers known BBVs including human immunodeficiency virus (HIV), hepatitis B virus (HBV) and hepatitis C virus (HCV). There are practical advantages in adopting common infection control policies to prevent the transmission of BBVs, and this is reflected in the guidance.
General principles
The BBVs which present most cross-infection hazard to HCWs are those associated with a carrier state with persistent replication of the virus in the human host and persistent viraemia. These include HIV and several hepatitis viruses, considered separately in the following paragraphs. For other rarer potentially blood-borne viruses, specialist virological advice should be sought.
In general, occupational risks of transmission of BBVs to HCWs arise from the possibility of exposure to blood and exceptionally to certain other body fluids or body tissues from an infected patient (see Table 1). Semen and breast milk may pose a risk of BBV infection but exposure of HCWs is considered unlikely in most healthcare settings.
Body fluids etc which should be handled with the same precautions as blood
- Cerebrospinal fluid
- Peritoneal fluid
- Pleural fluid
- Pericardial fluid
- Synovial fluid
- Amniotic fluid
- Semen
- Vaginal Secretions
- Breast milk
- Any other body fluid containing visible blood, including saliva in association with dentistry
- Unfixed tissues and organs
Human Immunodeficiency Virus (HIV)
HIV has been isolated from blood, semen, vaginal secretions, saliva, tears, urine, breast milk, and cerebrospinal, synovial and amniotic fluids. However only blood, blood products, semen, vaginal secretions, donor organs and tissues and breast milk have been implicated in the transmission of infection.
There is good evidence from studies of household contacts of infected people that HIV is not spread by close social contact even when this is prolonged, as in a family setting. A small number of cases of "household" transmission of HIV have occurred, but transmission is most likely to have occurred through exposure to infected blood or blood-contaminated body fluids.
Although HIV transmission may occur in health care settings, most HIV transmission occurs:
- by unprotected penetrative sexual intercourse with an infected person (between men or between man and woman);
- by inoculation of infected blood. At present in the UK this results mainly from drug misusers sharing blood-contaminated injecting equipment;
- from an infected mother to her baby before or during birth or through breastfeeding.
There is at present no vaccine to prevent HIV infection.
Hepatitis B virus (HBV)
Hepatitis B virus surface antigen (HBsAg) may be found in blood and virtually all body fluids of patients with acute hepatitis B and carriers of the virus but blood, semen and vaginal fluids are mainly implicated in the spread of HBV infection.
Transmission usually occurs:
- by unprotected sexual intercourse;
- by injecting drug misusers sharing blood-contaminated injecting equipment;
- perinatally from an infected mother to her baby.
Up to 90% of babies infected perinatally and around 5% to 10% of those infected as adults develop chronic carrier status. The persistence of the `e' antigen correlates with a high level of viral replication and increased infectivity. The most important measure whereby HCWs can be protected against HBV is by immunisation, which provides protection in up to 90% of recipients. Immunisation is not a substitute for good infection control practice since it provides no protection against infection with other BBVs.
Hepatitis C virus (HCV)
HCV is the main cause of what was previously known as non-A non-B hepatitis. HCV is most frequently acquired by direct blood to blood contact and the commonest mode of transmission in the UK is the sharing of blood contaminated injecting equipment by injecting drug misusers. Both sexual and perinatal transmission can occur but in general, these are less efficient modes of transmission. There is at present no vaccine to prevent HCV infection.
Hepatitis D virus (HDV)
HDV causes infection only in those who have active HBV infection. HDV infection can occur either as co-infection with HBV or as a superinfection of an HBV carrier. Since HDV depends on an HBV-infected host for replication, prevention of HBV infection by immunisation will also prevent HDV infection.
GB virus type C (Hepatitis G virus)
Recently a further BBV has been described, provisionally designated either as GBV-C agent or hepatitis G virus. The full clinical significance of infection with this virus, whether it is a true hepatotropic virus, and its natural history are as yet unknown.
RISKS OF TRANSMISSION OF BBVs
The risk of transmission of BBVs is greater from patient to HCW than from HCW to the patient. The risk to the HCW for each virus is proportional to the prevalence of that infection in the population served, the infectious status of the individual source patient, which may or may not be known, and the risk of a significant occupational exposure occurring during the procedures undertaken. In the healthcare setting transmission most commonly occurs after percutaneous exposure to a patient's blood by "sharps" or "needlestick" injury. The risk of transmission to a HCW from an infected patient following such an injury has been shown to be around 1 in 3 when a source patient is infected with HBV and is `e' antigen positive, around 1 in 30 when the patient is infected with HCV and around 1 in 300 when the patient is infected with HIV.
"Sharps" in this context are needles, sharp-edged instruments, broken glassware or any other item which may be contaminated in use by blood or body fluids and which may cause laceration or puncture wounds. Sharp tissues such as spicules of bone or teeth may also pose a risk of injury.
Most cases of occupationally acquired HIV infection have arisen from percutaneous exposure to HIV infected material, and of these, the majority have followed injury from hollow needles in association with procedures where a needle or cannula is placed in a vein or artery eg venepuncture. Others have arisen through exposure of mucous membranes or non-intact skin to blood.
Transmission of BBVs may result from contamination of mucous membranes of the eyes or the mouth, or of broken skin, with infected blood or other infectious material. The transmission risks after a mucocutaneous exposure are lower than those after a percutaneous exposure.

Doctors and students at a medical camp in Kenya.
The risk of acquiring HIV after a single mucocutaneous exposure is less than 1 in 2000. Mucocutaneous exposures occur more frequently than percutaneous exposure; the majority of both types of exposure are preventable.
BBVs are potentially transmissible by a human bite through mucous membrane exposure if the bite breaks the skin of the person bitten. There is no evidence that BBVs can be transmitted by blood contamination of intact skin, by inhalation or by faecal-oral contamination.
Not all patients infected with BBVs have had their infections diagnosed. It is therefore important that all blood and body fluids and tissues (see Table 1, page 9) are regarded as potentially infectious, and HCWs should follow precautions scrupulously in all circumstances to avoid contact with them.
PRECAUTIONS AGAINST EXPOSURE TO BBV INFECTION
Assessment of risk Health care staff carrying out clinical procedures should at all times carry out an assessment of the work to be done and of current procedures in order to be able to prevent or control exposure to substances hazardous to health.
Categorisation of risks and appropriate levels of protection
Each team or group of HCWs working together on a task should discuss the hazards involved in their current methods of working and ways of reducing these hazards. This process should include a consideration of the risks to others involved by such activities as the disposal of sharps, bodies, tissues, body fluids, and contaminated disposable items and the maintenance of equipment.
The team should be encouraged to devise safe and reasonably practicable procedures and routines for performing each task; ensure they are followed after appropriate training and keep them under active review.
The appropriate level of precautions to be taken for any procedure should be determined according to the extent of possible exposure to blood and not because of knowledge or speculation about the infectious status of the patient. All blood, tissues and some body fluids should be regarded as potentially infectious. This approach is sometimes referred to as "Universal Precautions."
General measures to reduce the risk of occupational exposure
- wash hands before and after contact with each patient, and before putting on and after removing gloves; change gloves between patients;
- cover existing wounds, skin lesions and all breaks in exposed skin with waterproof dressings3. Wear gloves if hands are extensively affected;
- wear gloves where contact with blood can be anticipated;
- avoid sharps usage where possible, and where sharps usage is essential, exercise particular care in handling and disposal;
- avoid wearing open footwear in situations where blood may be spilt, or where sharp instruments or needles are handled;
- clear up spillage of blood promptly and disinfect surfaces; wear gloves when cleaning equipment prior to sterilisation or disinfection, when handling chemical disinfectant and when cleaning up spillages;
- follow safe procedures for disposal of contaminated waste
HCWs should be encouraged to follow good practice methods. HCWs and their employers or supervisors should keep themselves informed of safe methods of working.
Safe handling and disposal of sharps Many percutaneous injuries are preventable. Such injuries may occur while hollow bore needles are being prepared for disposal, eg whilst attempting to resheath a needle manually after venepuncture. Implementation of the following procedures for the safe handling and disposal of sharps will reduce the risks:
- place all disposable sharps in sharps containers immediately after use. The containers should be placed safely out of reach of children as near as practicable to sites of use, be puncture resistant, of adequate depth and capacity and be suitable for incineration.
- provide sharps containers in adequate numbers and never overfill. They should be disposed of as clinical waste after closing securely, and replaced promptly;
- avoid resheathing needles manually. Only resheath needles if a device is available to allow this to be done using one hand only. If such a device is not immediately accessible, the single-handed scoop method may be used, i.e. the HCW holds the barrel of the syringe and scoops the needle cap from a hard, flat surface on to the end of the needle. Only when the needle tip is covered should resheathing be completed with the other hand. Resheathing devices should be decontaminated regularly;
- discard disposable syringes and needles wherever possible as a single unit, into sharps containers;
- remove needles from syringes only when essential eg when transferring blood to a container, or when the needle is disposable but the syringe is not, eg local anaesthetic syringes as used in dentistry. Needle forceps or other suitable devices should be readily available;
- remove needles and attach blind hubs to syringes containing arterial blood which are to be sent to the laboratory. Intravascular guidewires and glass slides must be disposed of as sharps.

We always require students to wear gloves and practice standard sanitary best practices.
GLOVES AND VENEPUNCTURE
Gloves cannot prevent percutaneous injury but may reduce the risk of acquiring a BBV infection. Although punctured gloves allow blood to contaminate the hand, the wiping effect can reduce the volume of blood to which the worker's hand is exposed and in turn, the volume inoculated in the event of percutaneous injury. Some HCWs with long experience of performing venepuncture without gloves may prefer not to wear them to avoid a perceived reduction of manual dexterity and possible consequent increased risk of percutaneous injury.
The following is advised:
- gloves are available to all HCWs who wish to wear them for venipuncture;
- inexperienced venepuncturists including medical students should become accustomed to the wearing of gloves from the beginning of their training, and should not take blood from patients known to be infected with BBVs until trained and considered competent;
- all venepuncturists, including those who are experienced, should wear gloves if there are cuts or abrasions on the hands and it is not practical for them to be covered by waterproof dressings alone, or if the patient is so restless that the risk of injury to the HCW is increased.
Reducing the risk of percutaneous exposure: methods, procedures and equipment The following measures may reduce the risk of percutaneous exposure and should be considered where practicable:
- have no more than one person working in an open wound/body cavity at any time (unless essential to the safe and successful outcome of an operation);
- use a "hands-free" technique where the same sharp instrument is not touched by more than one person at the same time, avoid hand to hand passing of sharp instruments during an operation;
- assure safer passage of necessary sharp needles and instruments via a "neutral zone", announce when a sharp instrument or needle is placed there. The "neutral zone" may be a tray, kidney basin or an identified area in the operative field;
- ensure that scalpels and sharp needles are not left exposed in the operative field, but always removed promptly by the scrub nurse having been deposited in the neutral zone by the operator or assistant;
- use instruments rather than fingers for retraction, and for holding tissues while suturing;
- use instruments to handle needles and to remove scalpel blades;
- direct sharp needles and instruments away from own non-dominant, or assistant's hand;
- remove sharp suture needles before tying suture; tie suture with instruments rather than fingers.
Alternative equipment and procedures should be considered where practicable:
- eliminate any unnecessary use of sharp instruments and needles, eg by appropriate substitution of electrocautery, blunt-tipped needles and stapling devices;
- opt for alternative less invasive surgical procedures where practicable and effective;
- avoid scalpel injuries associated with assembly/disassembly, by using scalpels which are either disposable, have retractable blades or which incorporate a blade release device;
- avoid the use of sharp clips for surgical drapes; blunt clips are available as are disposable drapes incorporating self-adhesive operating film;
- consider double gloving with a larger pair of gloves innermost for optimum comfort.
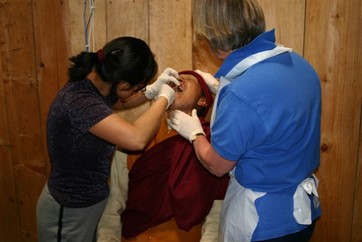
Students participating in a dental clinic in Nepal.
Reducing risk of blood-skin contact The following measures may reduce the risk of blood-skin contact and should be considered:
- if a glove puncture is suspected or recognised, rescrub if possible and reglove as soon as safety permits;
- change gloves regularly if performing, or assisting with a prolonged surgical procedure even if no glove puncture is suspected or recognised;
- the need for protection of body, eyes and face;
- choose waterproof gowns, or wear a surgical gown with waterproof cuffs and sleeves and a plastic apron underneath if blood contact and therefore "strikethrough" is considered a risk - such as procedures anticipated to involve high blood loss;
- if legs or feet may be contaminated (as in obstetric and some other procedures performed in the lithotomy position), ensure that impermeable gown/apron covers legs and wear impermeable footwear. Wellington or calf length overboots are preferable to shoes or clogs. Surgical drapes with "catch-basins" are available to reduce the risk of leg and foot contamination;
- wear protective headwear and surgical mask. Male HCWs should consider wearing hoods rather than caps to protect freshly shaven cheeks and necks; ensure that all blood is cleansed from a patient's skin at the end of an operation before patient leaves theatre;
- remove protective clothing including footwear on leaving the contaminated area. All contaminated reusable protective clothing, including footwear, should be subjected to cleaning and disinfection or sterilisation, with appropriate precautions for those undertaking it. Footwear should be adequately decontaminated after use.
MEASURES TO REDUCE EYE AND OTHER FACIAL EXPOSURE
Protect mucous membrane of eyes with protective eyewear. This should prevent splash injuries (including lateral splashes) without loss of visual acuity and without discomfort. Face shields may be considered appropriate for procedures which involve a risk of the splatter of blood including aerosols or other potentially infectious material. Various forms of combined eye and face protection are available Eyewash should be available in case of accidental exposure. Contact lenses should be removed prior to eye washing.
OTHER MEASURES TO PREVENT BBV TRANSMISSION
Hepatitis B immunisation
All HCWs, including students and trainees, who have direct contact with patient's blood or other potentially infectious body fluids or tissues should be immunised against HBV.
Decontamination and waste disposal
Many occupational exposures to BBVs result from failure to adhere to basic rules concerning decontamination, waste disposal etc. The following general guidelines should be drawn to the attention of all staff who come into contact with blood contaminated material. It is recommended that a member of senior management is designated as clinical waste control officer whose function it will be to oversee the operation of the clinical waste policy. This is particularly important in order to protect third parties, such as ancillary staff, and anyone else present in the healthcare setting, such as patients and their visitors, from preventable exposure.
Equipment and materials
Single-use equipment should be used where appropriate, particularly where decontamination cannot be carried out effectively. Any reusable equipment which is to be reused and which has been employed for a procedure involving potential contact with a patient's blood must be sterilised or disinfected before it is reused. Such equipment includes items which may not necessarily be in direct contact with the patient eg manual self-inflating resuscitation bags and dental handpieces. Reusable equipment must be of a type that is readily decontaminated without distortion or damage to its function. When selecting suction and aspiration equipment, apparatus which will discharge directly into a waste outlet is to be preferred in order to reduce the potential for accidental spillage.

Two student doctors stand outside of their clinic in rural Kenya.
Decontamination of equipment
Thorough physical cleaning of instruments in warm water with detergent to remove blood and debris is essential prior to disinfection or sterilisation, for either procedure to be effective. Neither cold nor hot water should be used for this purpose; the former may harden fats and the latter may cause the proteinaceous material to adhere.
Exposure Prone Procedures
are those where there is a risk that injury to the worker may result in the exposure of the patient's open tissues to the blood of the worker. These include procedures where the worker's gloved hands may be in contact with sharp instruments, needle tips and sharp tissues (spicules or bone or teeth) inside a patient's open body cavity, wound or confined anatomical space where the hands or fingertips may not be completely visible at all times.
Disposal of clinical waste
All waste which is contaminated with blood, tissues and other potentially infectious body fluids should be treated as "clinical waste", and disposed of following local protocols.
Management of blood exposure incidents
General principles
Needlestick and other exposures to blood in the healthcare setting are unnecessarily common at present. Many results from a failure to follow recommended procedures, and from careless disposal of waste. Strict adherence to the guidance earlier in this document should reduce the incidence of these exposures. There will remain occasions where exposure occurs despite careful attention to the correct procedures. All exposure incidents should be reviewed to consider how recurrence might be prevented. All HCWs in hospitals clinics and elsewhere (eg general medical and dental practice) should be informed and educated about the possible risks from occupational exposure and should be aware of the importance of seeking urgent advice following any needlestick injury or other possible exposure. Although the risk of acquiring a BBV through occupational exposure is low, the consequences are serious. Occupational exposure to known or suspected BBV infected material is always stressful, and for some, extremely so. HCWs, or any other person in the healthcare setting, exposed to HBV or HIV infected blood or body fluids should be offered appropriate post-exposure prophylaxis, if available and HCWs, particularly at risk of exposure to HIV, should be encouraged to consider in advance, whether in the event of an occupational exposure to HIV, they would wish to take prophylaxis.
At present, there is no effective post-exposure prophylaxis against HCV infection.
POST-EXPOSURE PROCEDURES
Action after an HCW has been exposed to blood or other potentially infectious body fluids should take account of the interests of both the worker and the source patient. The circumstances which led to the exposure should be identified and all possible steps are taken to prevent recurrence. Immediately following any exposure, the site of exposure ie. wound or non-intact skin should be washed liberally with soap and water but without scrubbing. Exposed mucous membranes including conjunctivae should be irrigated copiously with water, after first removing contact lenses if present. If there has been a puncture wound, free bleeding should be encouraged gently but the wound should not be sucked. HCWs who sustain an occupational exposure should report the exposure promptly and seek urgent advice on further management and treatment, from the senior doctor in their clinical setting.
Testing and counselling
The designated doctor (usually the supervising Doctor) will need, where possible, to obtain information from or about the source patient concerning possible indicators of BBV infection, including risk factors and results of previous tests for HIV and hepatitis, medical history suggestive of such infection; and details of past and current antiviral therapy in patients known to be HIV infected. The source patient should be asked to consent to testing for BBV infections including HIV, HBV and HCV. This will entail pre-test discussion and obtaining fully informed consent. If the source patient is approached in a sensitive manner, it is understood that consent to testing is rarely withheld.

A medical student helps a small family in Kenya get the treatment they need.
Post-exposure prophylaxis
HBV
If the HCW may have been exposed to HBV infected blood post-exposure prophylaxis should be considered, if available.
HCV
At present no post-exposure prophylaxis is available for HCV.
HIV
If the source patient is known to be infected with HIV or is considered to be at risk but has not been tested, health care workers are advised to attend the nearest accident and emergency department for urgent advice and possible post-exposure prophylaxis (PEP) treatment.
A designated doctor will be able to advise the healthcare worker of the risk of acquiring HIV infection after occupational exposure. Although post-exposure prophylaxis (PEP) is highly recommended, the UK recommended Anti Retroviral Medicines are not always readily available in developing countries, depending on your clinical setting and geographical location.
Post-Exposure Prophylactic (PEP) Antiretroviral Medicines will be available to all Adventure Alternative Medical Students whilst they are on a medical placement arranged by Adventure Alternative in Kenya, Tanzania or Nepal. The medicines will be purchased by Adventure Alternative staff locally following the current UK Department of Health recommendations.
Currently, the recommended medicines to be given as prophylaxis following exposure to bodily fluids deemed to be at high risk of HIV are:-
Zidovudine (AZT) 300mg - Twice a day for 7 days
Lamivudine (3TC) 150mg - Twice a day for 7 days
Nelfinavir 1250mg - Twice a day for 7 days
Decisions about prescribing these supplies of PEP will follow a risk assessment of the incident, based on the circumstances of the exposure and the source patient, under the guidance of the local supervising doctor.
The PEP will only be available to students whilst they are on placement. If a student wishes to carry a supply with them whilst on independent travel then they must purchase their own supply. The Adventure Alternative PEP starter pack will be kept in a central location within the Adventure Alternative Accommodation or within the hospital or clinic its f, so that it is readily available to all the students who may be on placement through Adventure Alternative at any one time. Please ensure you find out the location of the PEP from the local Adventure Alternative Representatives on arrival, before your placement commences.


